

Diabetic foot problems are more common than many people realise — and often misunderstood. For individuals living with diabetes, even a small foot issue can quietly worsen if not addressed early. Diabetic Footcare focuses on preventing complications, relieving symptoms, and protecting long-term mobility.
At Trinity Hospital and Heart Foundation, Basavangudi, diabetic footcare is approached as a preventive and restorative process, not just a reaction to wounds or ulcers. Under the care of Dr. Sravan C.P.S, patients receive structured evaluation and guidance aimed at preserving foot health and avoiding unnecessary procedures.
This treatment exists to help patients stay active, independent, and safe — without fear-driven decisions.
Diabetic footcare is a medical management plan designed to protect the feet from damage caused by long-term diabetes. High blood sugar can reduce blood flow and nerve sensation, making feet vulnerable to dryness, cracks, infections, blisters, swelling, or ulcers.
The goal of diabetic foot treatment is to:
It is not a single procedure, but a step-by-step care approach tailored to each patient's condition, lifestyle, and stage of diabetes.
Diabetic foot symptoms vary from person to person. You may benefit from medical evaluation if you notice:
Persistent diabetic feet swelling or diabetes swollen feet
Dry, cracked skin or diabetes dry feet
Numbness, tingling, or burning sensation in feet
Slow-healing wounds or diabetic foot blisters
Skin colour changes or temperature differences between feet
Diabetic foot ulcer symptoms — open sores or discharge, early signs in early stage diabetes feet
Nerve damage may reduce sensation — issues can progress silently without pain. Early and consistent care reduces complications.
Nerve damage may reduce sensation — issues can progress silently. Early detection and regular medical review are essential.
It is important to remember that diabetic foot problems can occur without pain due to nerve damage. Regular medical evaluation is essential.
See a doctor immediately if you notice redness, discharge, swelling, fever, non-healing wounds, or any new changes in foot sensation or appearance — even without pain.

Understanding what causes diabetic foot problems helps patients take preventive action and recognise early warning signs.
Reduced blood flow — poor circulation slows healing and increases infection risk
Nerve damage (neuropathy) — reduces sensation, making injuries go unnoticed
Poor footwear and pressure points — creates blisters, calluses, and ulcers
Dry skin and delayed wound healing — increases cracking and infection entry points
<strong>Types of diabetic foot conditions</strong> include dry/cracked feet, swelling, blisters, infections, and ulcers. In many cases, proper foot care and early intervention can prevent surgery and preserve mobility.
Diabetic foot treatment is always planned after careful assessment. Surgery is not the first step for most patients.
Non-surgical care may be advised when symptoms are mild to moderate or detected early. This may include:
Can proper foot care prevent surgery? In many cases, yes — early and consistent care significantly reduces complications and the need for intervention.
Regular follow-ups are crucial to track healing and prevent recurrence.
Surgical or interventional treatment may be considered if:
Intervention is recommended only when medically necessary, and always after discussing benefits, risks, and alternatives with the patient and family. The goal is limb preservation and functional recovery.
At Trinity Hospital and Heart Foundation, the focus is on targeted, limb-preserving interventions when surgery is required. The approach prioritises patient safety and long-term foot function.
Non-surgical diabetic foot care plan includes:
When surgical intervention is required:
This method is chosen to support safer recovery and long-term foot function in suitable cases.
At Trinity Hospital and Heart Foundation, diabetic footcare is supported by a multidisciplinary team and structured care pathways.
Facility includes:
EMI Options for Treatment:
Mediclaim & Insurance Support:
Blood sugar optimisation, structured wound care protocols, infection control, circulation-supporting medications, customised footwear, and medical-grade skin care. Regular follow-ups track healing and prevent recurrence. The goal is to detect problems early and avoid surgical intervention.
Specialised dressings, debridement of non-viable tissue, negative pressure wound therapy, and bioengineered skin substitutes. Used when conservative care alone is insufficient but surgical intervention is not yet required.
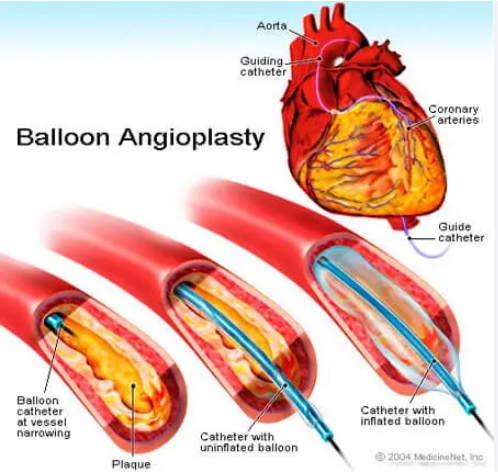
Minimally invasive endovascular procedures to restore blood flow to the foot when poor circulation is preventing wound healing. Performed by Dr. Sravan C.P.S using image-guided techniques. Supports healing and reduces amputation risk.
Surgical debridement, drainage of abscesses, and targeted removal of infected tissue when infection spreads to deeper structures. Coordinated multidisciplinary approach prioritises limb preservation. Method selection depends on foot condition, circulation status, infection severity, and overall health.
Diabetic footcare is about early action, informed decisions, and continuous care. Recovery and long-term management depend on ongoing commitment to foot health.
After treatment, patients should:
How often should diabetic patients check their feet?
Daily self-checks and regular medical reviews are recommended. This helps detect early changes before they progress to complications.

Diabetic footcare is about early action, informed decisions, and continuous care. A consultation with Dr. Sravan C.P.S at Trinity Hospital and Heart Foundation, Basavangudi helps determine:
What the consultation includes:
Medical guidance is always personalised — because every diabetic foot tells a different story.
Financial support available:
At Trinity Hospital and Heart Foundation, diabetic footcare is led by Dr. Sravan C.P.S with a focus on preventive care, early intervention, and limb-preserving approaches. Treatment is structured, evidence-based, and tailored to each patient's condition — with the goal of preserving mobility and independence.
Trinity Hospital and Heart Foundation, Bangalore
Dr. Sravan C.P.S is a consultant with focused experience in minimally invasive, image-guided treatments for vascular conditions including diabetic foot complications requiring vascular intervention.
His clinical approach emphasizes accurate diagnosis, patient education, and selecting treatment options based on individual symptoms rather than routine intervention. He believes that not all diabetic foot problems require immediate surgical treatment and prioritizes preventive care and wound management when clinically appropriate.
For patients requiring vascular intervention to improve foot circulation, Dr. Sravan is experienced in performing endovascular procedures using minimally invasive, image-guided techniques designed to restore blood flow and support wound healing.
Dr. Sravan is known for his clear communication style, helping patients and family members understand available treatment options and limitations, expected recovery and follow-up care, and practical steps for long-term foot protection.
At Trinity Hospital and Heart Foundation, he works within a multidisciplinary care framework — coordinating with endocrinology, wound care specialists, and infection control teams to ensure each patient receives evidence-based, ethical, and personalised treatment guidance.

Common questions and detailed answers about diabetic foot symptoms, treatment, prevention, and care
Reduced blood flow, nerve damage (neuropathy), poor footwear creating pressure points, dry skin, and delayed wound healing are common diabetic foot causes.
Yes. Nerve damage may reduce sensation significantly, so issues like ulcers or infections can progress silently without pain — making regular self-checks essential.
Daily self-checks are recommended, along with regular medical reviews. This helps detect early changes such as redness, swelling, or skin breaks before they progress.
Early-stage ulcers can heal with proper wound care, blood sugar control, and infection prevention. However, delayed treatment increases the risk of deeper infection and complications.
They include dry/cracked feet, swelling, blisters, calluses, infections, neuropathy (numbness), circulation problems, and ulcers ranging from early stage to advanced.
In many cases, yes. Early detection, consistent wound care, blood sugar optimisation, appropriate footwear, and regular medical monitoring significantly reduce complications and the need for surgical intervention.
Yes, when using doctor-recommended diabetes footcare moisturising lotion and avoiding application between the toes (which can trap moisture and increase infection risk).
Supportive, well-fitted footwear that reduces pressure points, has a cushioned sole, avoids tight areas, and protects feet from injury. Your doctor can provide specific recommendations.
If there is redness, discharge, swelling, fever, non-healing wounds, sudden colour change, foul odour, or any new changes in sensation or appearance — even without pain.
Yes. Ongoing care, regular medical reviews, daily self-checks, and blood sugar control help prevent recurrence and progression of foot complications.
Experiencing diabetic feet swelling, dry cracked skin, numbness, slow-healing wounds, or any diabetic foot symptoms? Schedule a consultation with Dr. Sravan C.P.S at Trinity Hospital and Heart Foundation, Basavangudi Bengaluru for expert, preventive diabetic footcare.
+91 8040136999
trinityheartfoundation@gmail.com
Trinity Hospital and Heart Foundation, Basavangudi, Bengaluru, Karnataka