

Repeat angioplasty is a specialised heart procedure offered when a previously placed stent starts narrowing again over time. At Trinity Hospital, Basavangudi, Bengaluru, this treatment is approached with care, caution, and a strong focus on understanding why the narrowing has occurred before deciding how to treat it.
Patients often come with concerns such as recurring chest discomfort, unexplained restlessness, or anxiety about whether their earlier stent is still working properly. Repeat angioplasty exists to address these situations thoughtfully—restoring blood flow while avoiding unnecessary intervention whenever possible.
Patients from Basavangudi, Jayanagar, JP Nagar, VV Puram, Banashankari, and NR Colony regularly consult for cardiac evaluation.
After a cardiac stent is placed, the artery usually remains open. However, in some patients, tissue can gradually grow inside the stent, leading to narrowing again. This process is medically called neointimal hyperplasia, and the resulting condition is known as stent restenosis or in-stent restenosis.
Repeat angioplasty is a treatment designed to manage this re-narrowing. The intent is not simply to redo a previous procedure, but to carefully evaluate the cause of restenosis and choose the safest, most appropriate solution for the individual patient.
Key principles at Trinity Hospital:
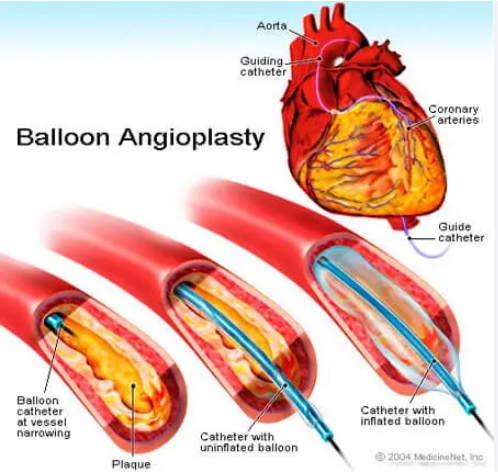
Symptoms of restenosis can be subtle and may resemble earlier heart-related complaints. These can include:
Chest pain or pressure, especially on exertion
Shortness of breath
Unusual fatigue or reduced exercise tolerance
Restlessness or discomfort without a clear reason
Reduced exercise tolerance
Not all patients experience the same symptoms, and some may notice only mild changes after a stent procedure. ECG alone may not always detect restenosis.
If symptoms recur after a stent procedure, consult a cardiologist—do not assume the cause.
It is important to remember that symptoms alone do not confirm restenosis. Proper clinical tests determine diagnosis.
If you have previously undergone stent placement and are experiencing recurring symptoms, or if test findings mention restenosis stent or cardiac stent ICD-10 classifications, a specialist consultation can help clarify the situation.

In-stent restenosis occurs when tissue grows back inside a previously placed stent, restricting blood flow.
Neointimal hyperplasia — tissue regrowth inside the stent
Uncontrolled diabetes, blood pressure, or cholesterol
Smoking and poor medication adherence
Stent type, size, or positioning factors
Understanding the specific cause and pattern of restenosis helps select the most appropriate repeat intervention or management approach.
Management of restenosis depends on symptom severity, test findings, and overall heart health. Treatment is never one-size-fits-all.
In selected cases, restenosis may be managed without immediate intervention:
Patients often ask: "How can I reduce my risk of developing restenosis?" Adherence to medication, regular reviews, and lifestyle changes play a significant role, especially in early or mild cases.
When symptoms persist or blood flow is significantly reduced, an interventional approach may be advised.
Repeat angioplasty is considered only after:
Decisions are made collaboratively—not automatically or under urgency.
At Trinity Hospital, Dr. B.G. Muralidhara focuses on precise assessment before choosing treatment for restenosis.
Primary Method: Repeat Angioplasty with Contemporary Stent Technologies
Drug-coated or everolimus-eluting stents may be recommended in suitable cases. These stents are designed to reduce the chance of excessive tissue regrowth inside the artery.
Other Available Methods:
The choice of method depends on factors like stent type, location, restenosis pattern, and the patient's overall health. The emphasis is always on safety, long-term vessel health, and recovery—not on routine re-intervention.
Accurate diagnosis and treatment of in-stent restenosis requires specialized catheterization laboratory capabilities.
The facility includes:
At Trinity Hospital and Heart Foundation, the evaluation includes careful review of prior angioplasty reports, current imaging, and clinical assessment before any treatment decision is made.
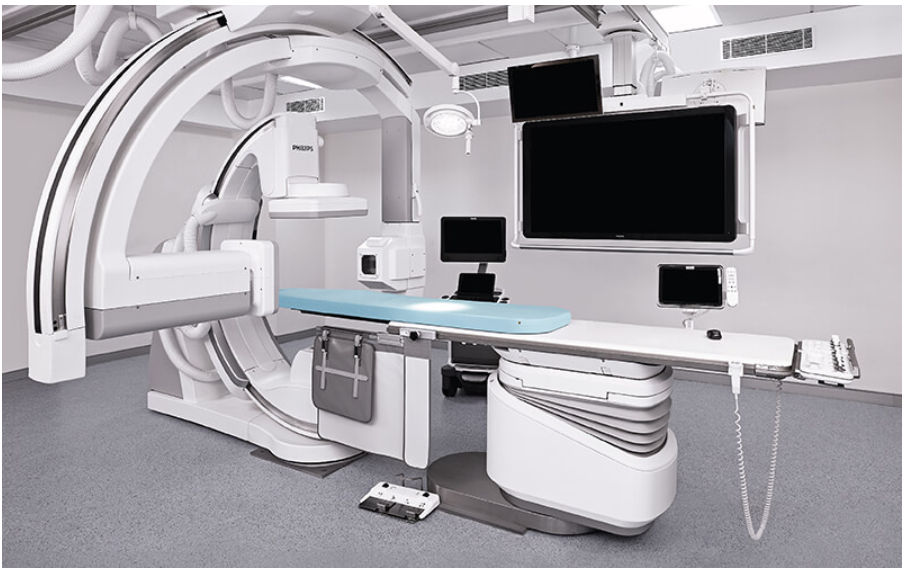
Using contemporary stent technologies including drug-coated or everolimus-eluting stents, designed to reduce the chance of excessive tissue regrowth. Recommended in suitable cases after careful assessment of the existing stent condition.
A balloon coated with anti-proliferative drug is used to open the re-narrowed stent and deliver medication directly to the vessel wall, helping prevent further tissue regrowth without placing an additional stent.
In selected cases, balloon dilation alone may be appropriate depending on the restenosis pattern, stent condition, and overall vessel anatomy. Advanced imaging guides the approach.
For mild or early restenosis, optimised medical therapy including blood pressure control, cholesterol management, diabetes control, and lifestyle modification with close follow-up may be sufficient.
Recovery after repeat angioplasty is similar to the initial procedure, with focused attention on preventing future restenosis.
Recovery and follow-up includes:
Taking prescribed medications regularly, controlling blood pressure and diabetes, avoiding smoking, following dietary advice, and attending follow-up appointments can help reduce the risk of further restenosis.

If you have previously undergone stent placement and are experiencing recurring symptoms, or if you are unsure about test findings such as reports mentioning restenosis stent or cardiac stent ICD-10 classifications, a specialist consultation can help clarify the situation.
The consultation at Trinity Hospital focuses on:
Location & Care Access:
Trinity Hospital, Basavangudi, Bengaluru. Patients from nearby areas and referred cases are evaluated with continuity of care, ensuring prior records and reports are carefully reviewed.
Repeat angioplasty is not always the first or only answer. The focus is on choosing the right solution at the right time, guided by patient safety, clinical evidence, and informed decision-making.
Dr. B. G. Muralidhara evaluates patients with in-stent restenosis and provides guidance on the most appropriate treatment approach—whether repeat intervention or optimised medical management.
Trinity Hospital and Heart Foundation, Bangalore
Dr. B. G. Muralidhara has extensive clinical experience of 30+ years in managing heart conditions and has been involved in the evaluation and treatment of a large number of patients with coronary artery disease including complex restenosis cases.
His clinical work includes diagnostic angiography and angioplasty procedures, along with long-term cardiac care planning. Patients often consult him for clear explanations, second opinions, and guidance on whether repeat angioplasty is necessary or if medical management is sufficient.

Common questions and detailed answers about stent restenosis and repeat angioplasty
Restenosis refers to the re-narrowing of an artery at the site where a stent was previously placed. It usually happens due to tissue growth inside the stent, a process called neointimal hyperplasia.
In-stent restenosis specifically means narrowing that occurs within the stent itself. This can reduce blood flow and may cause symptoms similar to those experienced before the original angioplasty.
Some patients experience restlessness due to reduced blood flow, anxiety, medication effects, or changes in heart function. Restlessness alone does not confirm restenosis and should be evaluated by a cardiologist.
Symptoms may include chest discomfort, shortness of breath, fatigue, reduced exercise capacity, or unexplained restlessness. Symptoms vary widely and may be mild in some patients.
An ECG can show signs of reduced blood flow, but it cannot reliably confirm restenosis on its own. Additional tests such as imaging or angiography may be required based on clinical evaluation.
Repeat angioplasty is a procedure used to treat narrowing that has developed again inside or near a previously placed stent. It is considered only after careful assessment of symptoms and test results.
No. Some cases can be managed with medications, lifestyle changes, and close monitoring. Repeat angioplasty is recommended only when non-surgical options are insufficient or symptoms persist.
Taking prescribed medications regularly, controlling blood pressure and diabetes, avoiding smoking, following dietary advice, and attending follow-up appointments can help reduce the risk of restenosis.
Depending on the case, drug-eluting stents such as everolimus-eluting stents or drug-coated balloon technologies may be used. The choice depends on artery condition and prior treatment history.
If you notice recurring symptoms, changes in exercise tolerance, or have concerns about test reports mentioning restenosis or cardiac stent classifications, it is advisable to consult a cardiologist for evaluation.
If you're experiencing recurring symptoms after a previous stent procedure, consult with Dr. B.G. Muralidhara at Trinity Hospital, Basavangudi Bengaluru for comprehensive evaluation and guidance.
+91 8040136999
trinityheartfoundation@gmail.com
Trinity Hospital and Heart Foundation, Basavangudi, Bengaluru, Karnataka